|
TABLE OF CONTENTS HIGHLIGHTS INTRODUCTION HCUP PARTNERS 1. OVERVIEW 2. DIAGNOSES 3. PROCEDURES 4. COSTS 5. WOMEN'S HEALTH SOURCES/METHODS DEFINITIONS FOR MORE INFO ACKNOWLEDGMENTS CITATION FACTS & FIGURES 2009 PDF |
EXHIBIT 4.5 Cost by Diagnostic Category (PDF) 4.5a 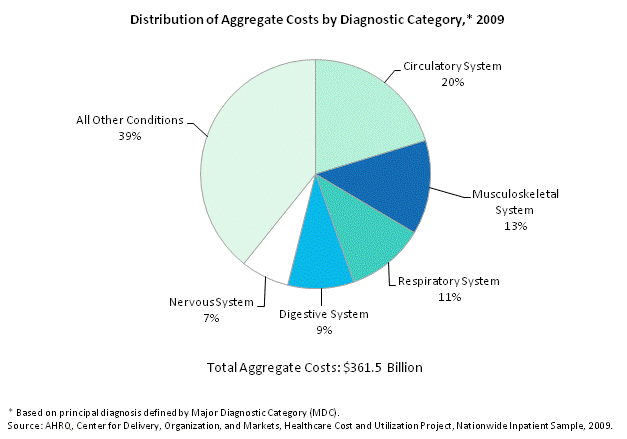
Distribution of aggregate costs by diagnostic category, 2009. Pie chart. Circulatory system: 20%; Musculoskeletal system: 13%; respiratory system: 11%; digestive system: 9%; nervous system: 7%; all other conditions: 39%. Total aggregate costs: $361.5 billion. Note: Diagnostic categories are based on principal diagnosis defined by Major Diagnostic Category (MDC). Source: AHRQ, Center for Delivery, Organization, and Markets, Healthcare Cost and Utilization Project, Nationwide Inpatient Sample, 2009.
4.5b
Costs by diagnostic category varied by payer, as did the distribution of costs.
4.5c 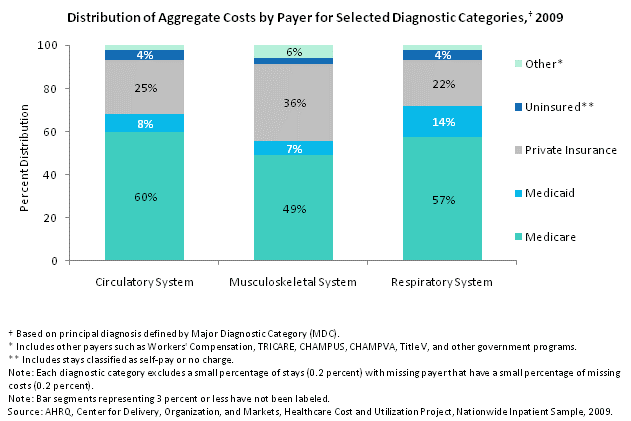
Distribution of aggregate costs by payer for selected diagnostic categories, 2009. Column chart. Percent distribution. Circulatory system. Other: 2%; uninsured: 4%; private insurance: 25%; Medicaid: 8%; Medicare: 60%. Musculoskeletal system. Other: 6%; uninsured: 3%; private insurance: 36%; Medicaid: 7%; Medicare: 49%. Respiratory system. Other: 3%; uninsured: 4%; private insurance: 22%; Medicaid: 14%; Medicare: 57%. Note: Diagnostic categories are based on principal diagnosis defined by Major Diagnostic Category (MDC). Note: Other includes other payers such as Workers' Compensation, TRICARE, CHAMPUS, CHAMPVA, Title V, and other government programs. Note: Uninsured includes stays classified as self-pay or no charge. Note: Each diagnostic category excludes a small percentage of stays (0.2%) with missing payer that have a small percentage of missing costs (0.2%). Source: AHRQ, Center for Delivery, Organization, and Markets, Healthcare Cost and Utilization Project, Nationwide Inpatient Sample, 2009.
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Internet Citation: Facts and Figures 2009. Healthcare Cost and Utilization Project (HCUP). November 2011. Agency for Healthcare Research and Quality, Rockville, MD. hcup-us.ahrq.gov/reports/factsandfigures/2009/exhibit4_5.jsp. |
| Are you having problems viewing or printing pages on this website? |
| If you have comments, suggestions, and/or questions, please contact hcup@ahrq.gov. |
| If you are experiencing issues related to Section 508 accessibility of information on this website, please contact hcup@ahrq.gov. |
| Privacy Notice, Viewers & Players |
| Last modified 11/9/11 |